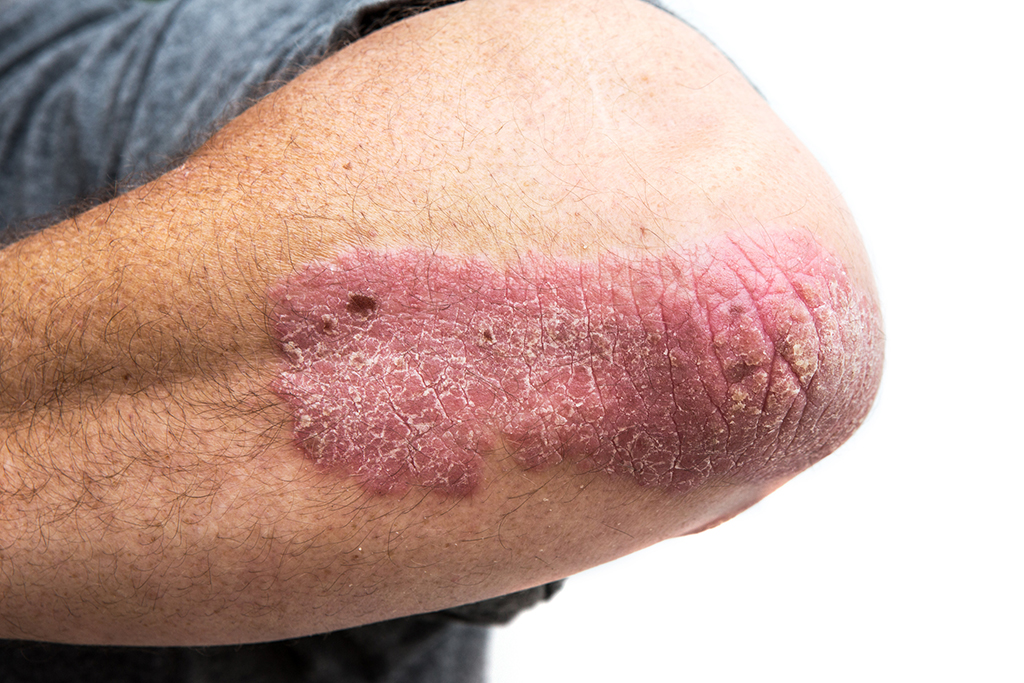
Photo By JodiJacobson at istock
Dermatologists are not always the first medical professionals that come to mind when we think of autoimmune diseases. Perhaps that line of thinking should be altered. They have a very important role in diagnosing autoimmune illnesses, and they’re often the first medical professionals to notice potential warning signs.
What Are Autoimmune Illnesses?
Many autoimmune illnesses affect the skin, and the skin is frequently the first organ to show symptoms. Approximately 5% of the population is affected by an autoimmune illness. These illnesses are more common in women, and people with a family history are at higher risk of developing an autoimmune illness themselves.
Diseases are characterized as ‘autoimmune’ when they are caused by the immune responses that should protect our bodies from illness and heal injuries. These immune responses overreact and target healthy skin, connective tissues, and organs.
Autoimmune Skin Disorders
Dermatologists in Southlake, TX, and the rest of the nation, are often the first doctors to identify and manage individual cases of autoimmune skin disorders including, dermatitis herpetiformis, pemphigoid, pemphigus, and vasculitis.
Autoimmune diseases affecting connective tissue include lupus erythematosus, dermatomyositis, and scleroderma. Symptoms present in different ways for each person. Common symptoms include rashes, sensitivity to sunlight, sores around the mouth, hair loss, and changes in the nails.
Sometimes people with these illnesses only develop symptoms affecting the skin, while others have symptoms affecting internal organs as well. Skin changes almost always occur first.
Dermatologists perform comprehensive skin examinations to find early signs and symptoms of autoimmune connective tissue diseases. Laboratory tests and skin biopsies help confirm diagnosis and find signs of problems with internal organs.
Rheumatoid diseases, such as rheumatoid arthritis, can also affect connective tissue. A common blood test detects an autoantibody called the rheumatoid factor. This test is very important because a tentative correlation exists between levels of the rheumatoid factor in blood and severity of the condition. A positive test provides a warning of potential systemic involvement or complications.
Autoimmune Blistering Diseases
Autoimmune blistering skin diseases occur when the immune system attacks proteins in the skin that hold layers of skin together. Painful blisters form on the skin and mucous membranes when those proteins are damaged or depleted. A dermatologist can usually differentiate between blisters caused by burns or injuries and blisters signifying autoimmune disease in a relatively short time.
Autoimmune blisters occur over larger areas of the body and heal much more slowly than blisters resulting from burns and injuries. Both types may cause scarring, but scarring is more extensive with autoimmune blisters.
Autoimmune blistering diseases occur in men and women equally and usually appear after age 50, although they can occur in people of all ages.
Autoimmune blistering skin diseases include pemphigus, pemphigoid, IgA-mediated bullous dermatoses, and epidermolysis bullosa acquista. These diseases often present with very similar symptoms, but there are some differences a dermatologist recognizes.
Symptoms occur on different areas of the body and manifest in different ways according to each disorder. Pemphigus causes erosion and sores in the mouth, throat, nose, eyes, scalp, or genitals. Pemphigoid is an umbrella term for several disorders that cause fluid-filled blisters, erosions, and sores on the skin and mucous membranes.
IgA-mediated bullous dermatoses also includes a group of disorders that causes blisters on the skin and mucous membranes. Epidermolysis bullosa acquista causes blisters too, but skin also becomes noticeably more fragile and loses elasticity.
Other symptoms of these illnesses include mouth pain, difficulty breathing, difficulty swallowing, bleeding in the digestive tract, and problems with vision. Treatment is a combination of corticosteroids, anti-inflammatory medications, and immuno-suppressing drugs.
Dermatologists diagnose blistering autoimmune diseases with a complete evaluation. It begins with a physical exam, review of personal and family medical history, and a discussion of symptoms.
Several diagnostic tests are used to support, confirm, or dismiss a diagnosis. Blood draws generally check for disease- specific autoantibodies. In the case of blistering diseases, the tests look for immune proteins in the skin or proteins that attack the skin.
A dermatologist performs a skin biopsy by removing a small sample of affected skin and examining it under a microscope. Direct immunofluorescence is performed on a small sample of unaffected healthy skin to identify a person’s normal immune proteins. Determining the healthy state of a person’s skin helps understand disease progression.
Treatment
Medical teams treating autoimmune illnesses often include a dermatologist, several doctors in other fields, and physical or occupational therapists. A team of professionals in different fields is valuable because these illnesses can cause symptoms affecting many different parts of the body.
Medications are used to manage symptoms and treat the underlying causes. Doctors monitor symptoms, medication side effects, and systemic manifestations to determine the most effective combination of medication and interventions.
It is important to note that most autoimmune disorders are chronic conditions. Remission can last anywhere from days to years, but autoimmune disorders can not actually be cured through medical science yet.
Topical ointments, creams, and lotions are common treatments. Some dermatologists recommend light therapy to relieve rashes and itching. Laser treatment is a fairly new procedure. They uses a highly-targeted medical laser to address affected areas on the skin.
Vitamins are a staple of treatment regimes because they help the body fight the underlying autoimmune condition. Extreme cases of scleroderma may be treated with surgical amputation or transplants.
The causes of autoimmune blistering diseases are not well understood and usually have a genetic component, but certain factors can cause outbreaks and worsen symptoms. Common triggers include specific foods, medications for high blood pressure or diabetes, antibiotics, and exposure to ultraviolet light.
The field of dermatology is much, much more than cosmetic procedures. It is a vital component of the complex health care infrastructure that helps us live healthy, happy lives. Make sure to schedule an appointment with Compassion Dermatology in Southlake, TX, even if you feel fine. Early diagnosis is beneficial and contributes to positive treatment outcomes for any autoimmune disorder, and most medical conditions in general.


